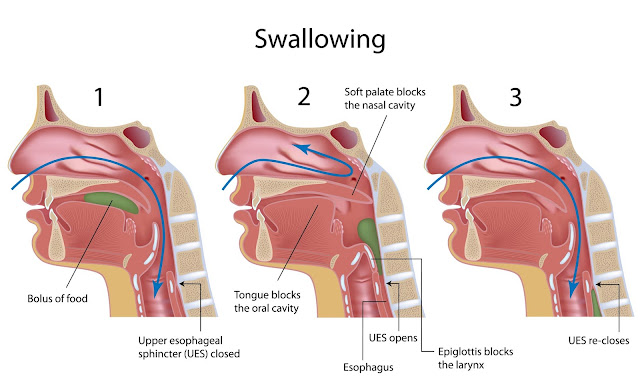
The danger of swallowing disorders is that they can lead to aspiration pneumonia and poor nutrition. Both conditions contribute to declining health and increased length of hospital stays. Symptoms of difficulty swallowing include:
- coughing
- choking
- food "sticking in the throat"
- drooling
- nasal drainage while eating
- weight loss
- fever from pneumonia
The Diagnosis of Dysphagia
When the above symptoms are noted by physicians, nurses or therapy staff, a speech-language pathologist (SLP) is consulted. Patients hospitalized for neurological disorders such as stroke, brain injury, Parkinsonism, or ALS likely are on the SLP caseload.Swallowing requires timely and effective coordination of many muscles. When these do not operate efficiently, ingested substances can enter the airway and endanger patient health.
After the referral, an evaluation takes place. The SLP offers different food textures to assess difficulty swallowing them separately. Liquids, pudding, crumbling foods such as crackers and sometimes more complex foods containing mixed textures are introduced. The SLP assesses the patient's ability to:
- chew (masticate) food thoroughly
- clear food from pockets in the mouth
- form a bolus (food ball)
- use the tongue to project the bolus toward the pharynx
- maintain timeliness and coordination of oral and pharyngeal movements to keep food on track
- maintain timeliness of elevation of the larynx (Adam's apple area)
- clear residual food from pockets around the airway (valecula)
- move the epiglottis to cover the airway
- effect travel of the ingested material down the esophagus
Assessments begin at bedside with behavioral observations. In addition to bedside evaluation, the SLP can perform tests such as a modified barium swallow study (MBSS) or a fiberoptic endoscopy study (FEES). The MBSS uses barium, a white substance that shows up on X-ray, indicating the path of ingested material. The FEES uses a camera above the vocal cords and color-tinted food, so the SLP can assess efficiency of food transfer.
These tests also help determine whether there is "silent aspiration." Liquids especially can penetrate into the airway, without coughing, in serious cases of impairment. When patients say they have no trouble at all with liquids, there can still be a dangerous problem.
Treatment of Swallowing Disorders
After determining the nature of the problem, several approaches may come into play. With silent aspiration, or in very severe cases of dysphagia where management is not immediately possible, feeding tubes may be necessary. A nasogastric tube (from the nose to the stomach) or a PEG (percutaneous endoscopic gastrostomy) tube may be placed to provide nutrition until the patient's condition improves.The following treatments may be appropriate for specific patients:
- Diet: easy to chew if oral problems occur
- Thickened liquids when thin consistencies are difficult to manage
- Sit upright for at least 20 minutes after ingesting anything
- Small bites and sips to make it easier to manage
- Slowed intake
- Provide assistance when needed, especially if the patient is fatigued
- Oral exercises to increase strength and range of motion (ROM) of the tongue
- Lip strengthening exercises to improve lip seal and avoid leakage
- Exercises to increase laryngeal strength